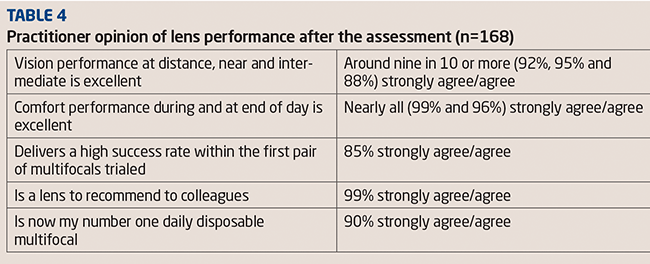
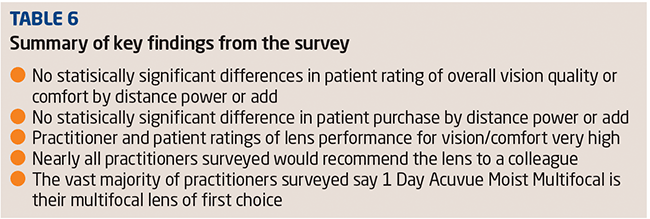
In this article I will discuss two case studies concerning the first two patients I fitted with orthokeratology lenses plus a sequence of topography images from a patient who decided to stop wearing orthokeratology (ortho-k) lenses.
After returning from the course run by one of my lens suppliers, I was keen to try out the lenses but preferably on someone I knew so I could more easily keep a close eye on the results. Luckily, I had two trainee dispensing opticians in my store who were both very keen to try ortho-k correction. They were also the only myopes in store with prescriptions in the recommended range.
Case study 1 — KS
KS was a 21-year-old myope who wore spectacles at work and daily disposable contact lenses for playing sport and socially. She was a semi-professional tennis player and coach. She occasionally forgot to put lenses in her tennis bag and therefore had to play wearing her spectacles. Being correction-free during the day would therefore be of benefit as she would not have to remember to take her lenses with her.
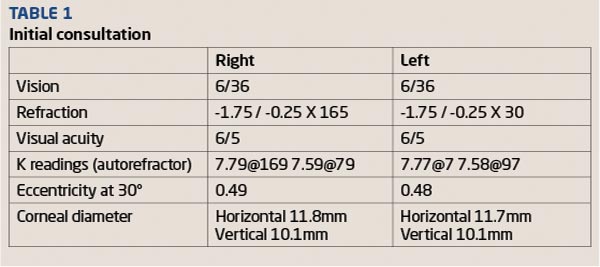
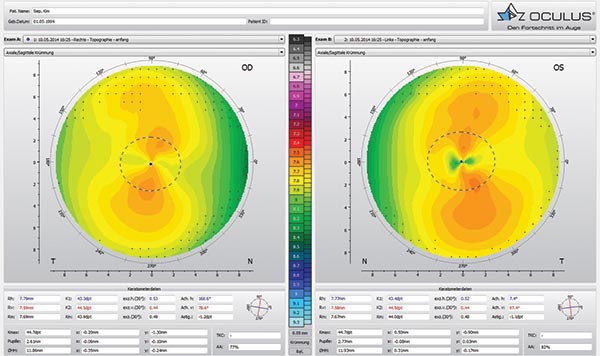
Initial consultation data is shown in Table 1 and the initial topography results are shown in Figure 1.
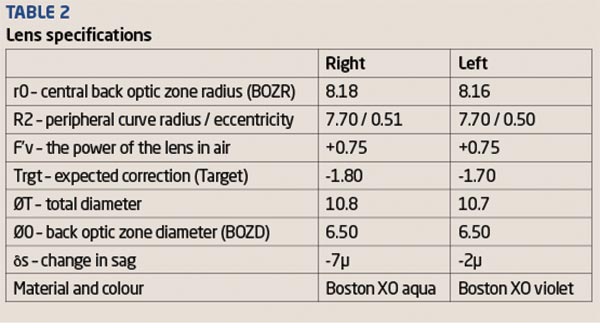
Slit lamp examination showed nothing unusual. The lenses were ordered by sending the topography pictures and the initial consultation data by e-mail to one of my RGP lens suppliers. The lenses arrived within a week and had the specifications shown in Table 2.
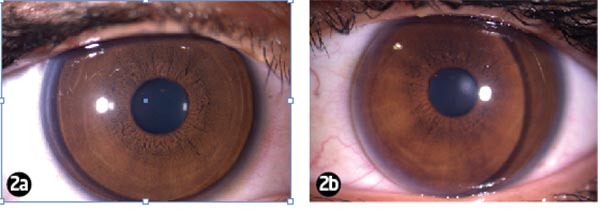
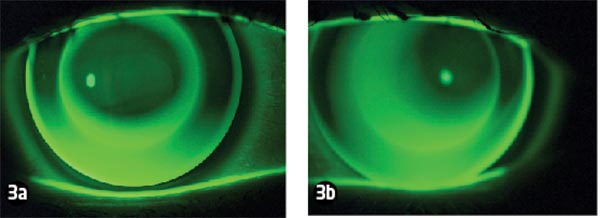
The lenses were inserted using Boston Advance Conditioning Solution to ensure there were no air bubbles captured (initial appearance and fluorescein pattern are shown in Figures 2 and 3 respectively) and were then worn for an hour. During this time KS reported the usual initial RGP discomfort, reporting the lenses to be rubbing on the lids and some irritation during ocular movement and blinking. Her vision was, however, clear (6/6 R and L).
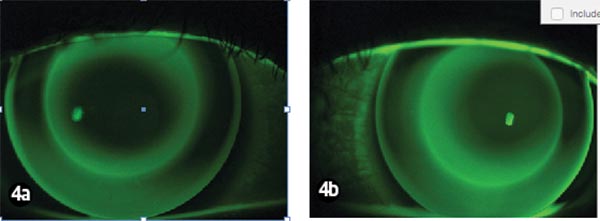
After an hour, the lenses were assessed for fit with and without fluorescein on the slit lamp. KS then had to learn how to remove the lenses because this was her first RGP fitting. After removal a new topography picture was taken (Figure 4). This already showed some central flattening and mid-peripheral steepening although it was not regular or concentric.
We then cleaned the lenses using Boston Advance daily cleaner, rinsed them with saline and placed them into AOSept to disinfect so they would be ready for the evening. KS was instructed to insert them, using Boston Advance conditioning solution, about 30 minutes before going to bed, and to leave them in until she got to work in the morning. She was also asked to bring the solutions and case with her so they could be cleaned after her first aftercare appointment.
First aftercare
The next morning, KS came to work wearing the lenses and reported that her vision with the lenses was good. She had experienced some initial discomfort on inserting the lenses and she felt it had taken her a little longer to get to sleep than normal. She could not say whether that was due to some discomfort or because she was thinking about having the lenses in her eyes and worrying about them moving while she slept.
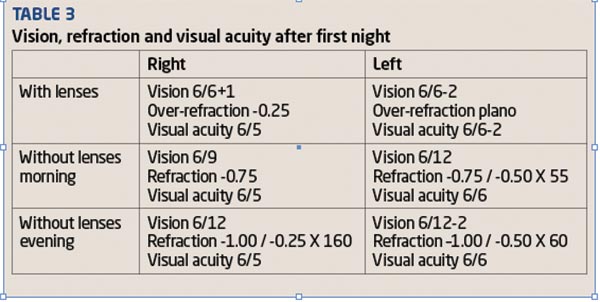
The vision, over-refraction and visual acuity were checked with the lenses in situ (see results in Table 3). The lens fitting was then assessed using the slit lamp with and without fluorescein (Figure 4). The lenses were found to be adequately mobile to be removed without lid massage. KS removed the lenses and placed them temporarily in the case so we could complete the aftercare.
Next, the vision, refraction and visual acuity were assessed without the lenses (see Table 3) and then topography pictures taken (Figure 5). KS was happy with her initial vision but to ensure she could see clearly she used Focus Dailies Total 1 lenses (-0.75 R and L) for the rest of the day.
[CaptionComponent="2035"]Because she was in store the whole day, we decided to also check her vision, refraction and visual acuity at the end of the day (see Table 3). This is not something that would normally be done because it requires too many appointments for the patient and practitioner. KS then cleaned the lenses as instructed and placed them in AOSept so they would be ready to wear in the evening.
Subsequent aftercares
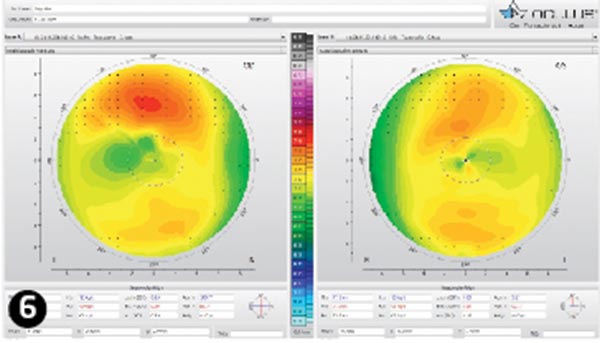
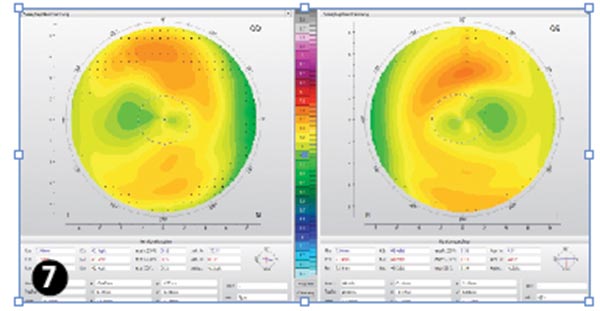
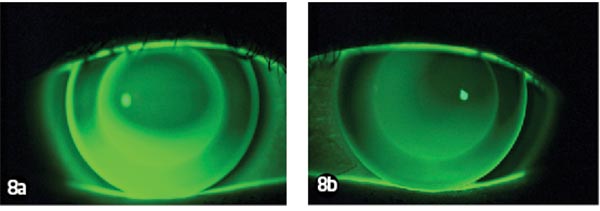
The next aftercares followed a similar pattern except that KS attended without wearing the lenses, though always bringing them with her. Aftercares took place after four nights (Figure 6), nine nights (Figures 7 and 8) and one month (Figure 9). After five nights she stopped using daily disposable lenses during the day because she felt her vision was adequate during the day and she used public transport to travel home after work. The results are shown in Table 4.
During the first month, KS said she did have some difficulties with haloes when driving at night. After nine nights, I discussed this with the lens supplier who advised that KS should continue wearing the initial lenses for at least one month before any changes to the fitting be made. Often, epithelial migration is not complete in the early weeks and this can lead to a smaller effective optic zone. Hence haloes can be seen at night when the pupil diameter is bigger.
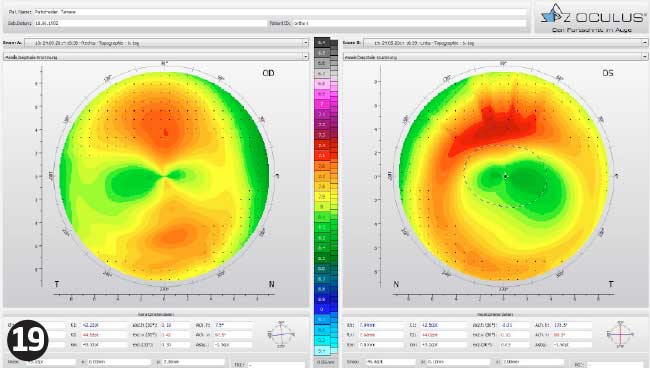
After six weeks, although the vision was excellent, regression minimal, central flattened zone well-centred and no correction required during the day, KS was still experiencing haloes and the decision was made to change the lenses. Information about vision, over-refraction, visual acuity and fitting of the lenses plus up-to-date topography pictures were sent to the supplier so it could make the required modifications to the lens specifications.
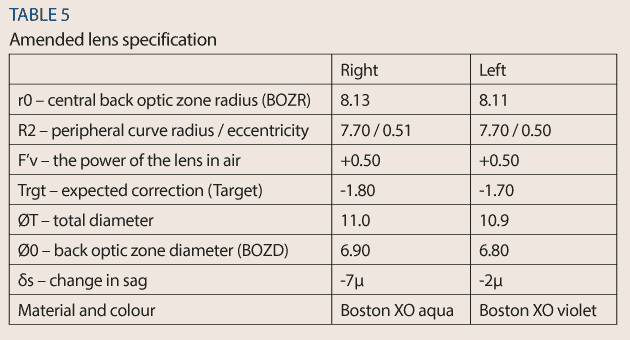
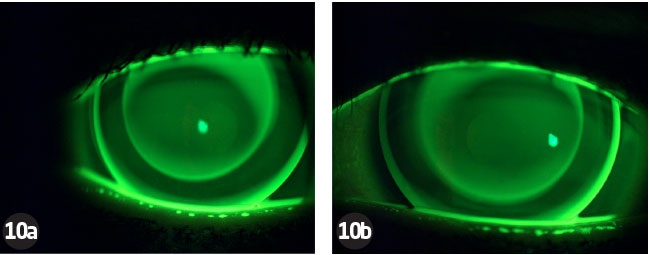
The back optic zone diameter (BOZD) and total diameter were made larger in the hope that the effective optic zone would become larger, reducing the chance of getting haloes at night (Figure 10). The new specification is shown in Table 5.
These new lenses were then worn at night, as previously, and within two weeks KS noted that the haloes had disappeared. It was only when I asked if she had noticed a difference that she told me they were no longer there. The change in the effective optic zone diameter was minimal but was enough to make it bigger than the mesopic pupil diameter. KS was happy with her vision throughout the day and delighted that she could now enjoy playing tennis without having to worry whether she had packed her daily disposable lenses.
After six months of problem-free wearing, KS decided that she missed having the option of wearing spectacles and reverted to wearing them while working and lenses for sport. She was pleased to have been given the opportunity to try ortho-k and happily recommends it to patients and friends.
Case study 2 — TP
TP was a 23-year-old myopic trainee dispensing optician. She normally wore monthly disposable contact lenses during the day and spectacles in the evening and occasionally at the weekend. She was happy with her lenses but not with not being able to see in the mornings. She had considered laser eye surgery but the cost in Switzerland was prohibitive for her. She was keen to try the ortho-k lenses so she might not be so reliant on her glasses, especially on first waking.
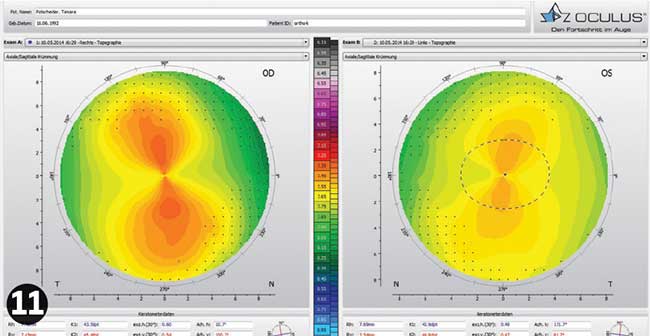
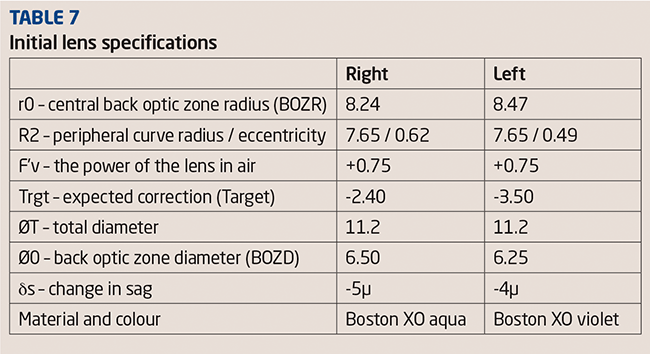
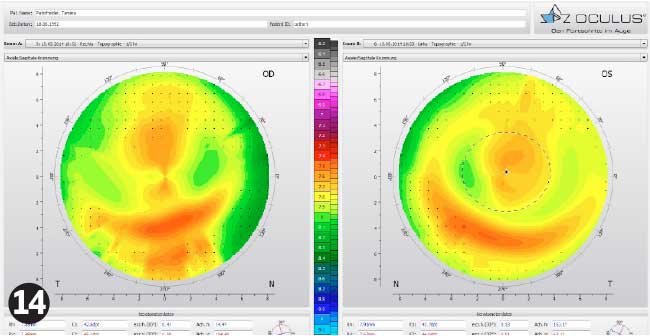
Initial consultation data is summarised in Table 6 and the initial topography shown in Figure 11. Slit lamp examination showed nothing unusual. The lenses were ordered by sending the topography pictures and the initial consultation data by e-mail to an RGP lens supplier. The lenses, with the specifications summarised in Table 7, arrived within a week.
It is interesting to note the difference in BOZR and BOZD between the lenses due to the anisometropia. The expected effective optic zone is smaller and flatter in the left eye than the right eye. Luckily, TP had smaller pupils than KS.
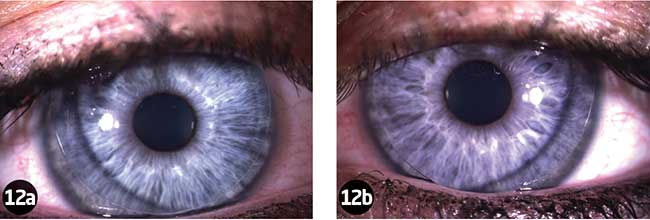
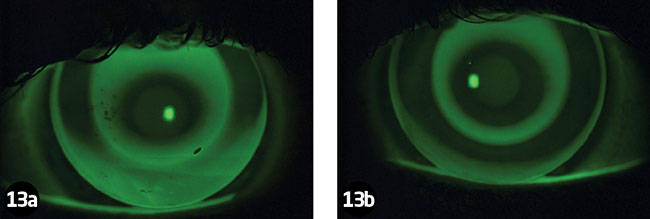
The lenses were inserted using Boston Advance conditioning solution so that there were no air bubbles under the lenses. The lenses were then worn for one hour so I could better assess the fit. During this time she said she had a foreign body sensation in both eyes but it was tolerable and she did not feel the need to remove the lenses. She also noted that comfort improved when she kept her eyes closed. The lenses were then assessed on the slit lamp with and without fluorescein (Figures 12 and 13).
The lenses centred well and the typical ring pattern could already be seen. TP then removed the lenses and cleaned them with Boston Advance daily cleaner, rinsed them with saline and placed them in AOSept so they would be ready to insert in the evening. A topography picture was then taken (Figure 14). It already showed a change in corneal shape and TP commented that her spectacles felt ‘too strong’ when she put them back on again.
TP was instructed to put the lenses in about 30 minutes before going to bed and to come to work in the morning with the lenses still in place. She was also asked to bring the solutions and her contact lenses case with her.
First aftercare
TP arrived at work in the morning wearing her lenses and had worn them for about 11 hours. She said she had barely noticed them in her eyes when she was trying to get to sleep and her only concern was what would happen if she rolled onto her face during sleep. She felt her vision was as clear as when wearing her usual monthly lenses.
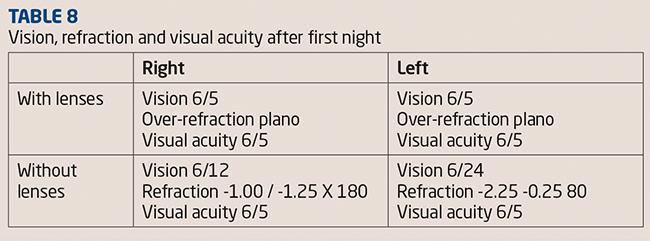
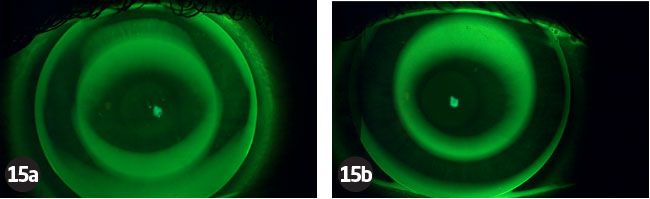
The vision, over-refraction and visual acuity were checked with the lenses in situ (see Table 8). The lens fitting was then assessed using the slit lamp with and without fluorescein (Figure 15).
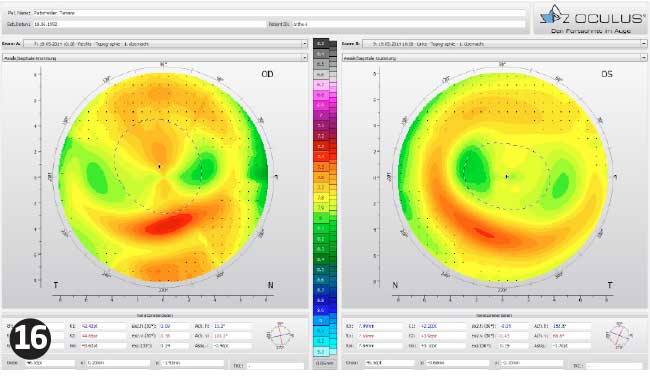
The lenses were found to be adequately mobile to be removed without lid massage. TP removed the lenses and placed them temporarily in the case so we could complete the aftercare. The topography data is shown in Figure 16.
Because there was still a significant refraction TP was given Focus Dailies Aquacomfort Plus lenses (R -1.00 -1.25 X 180; L -2.25DS) to wear for the rest of the day. She was pleased with the initial vision but the lenses did not have as much of a ‘wow’ effect on her as they had KS.
TP then cleaned the lenses as instructed and placed them in AOSept so they would be ready to insert in the evening.
Subsequent aftercares
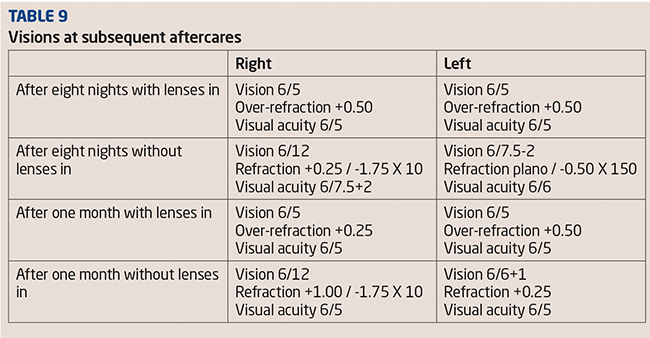
In TP’s case, due to her work schedule and holiday, we were only able to complete follow up aftercares after eight nights and one month. During this time she ‘self-checked’ her refraction and used daily disposable lenses as necessary. The results of these aftercares are shown in Table 9.
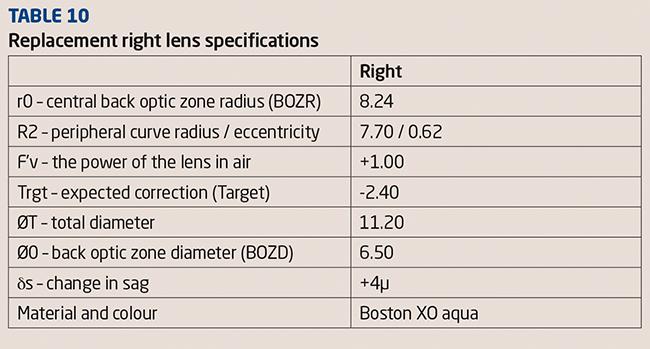
As can be seen from the results the left eye reacted well to the lens wear and most of the correction was removed within the first week. After this time TP felt no need to wear daily disposable lenses in her left eye during the day. However, the right eye had a stubborn horizontal cylinder that would not go away. At the one-month aftercare a new lens was ordered for the right eye in the hope of correcting the astigmatism better (see Table 10).
This new lens was then worn for 10 nights but the astigmatism was still present. TP continued to wear the new lens for a month as recommended by the supplier. The refraction after 10 nights and at the end of the month can be seen in Table 11.
At the end of the month the astigmatism was still present and, during the day, required correction with daily disposable lenses, although TP’s dominant eye is her right one. It was decided we would try a different supplier who could make an ortho-k lens with a toric periphery claimed to correct astigmatism up to -2.50DC.
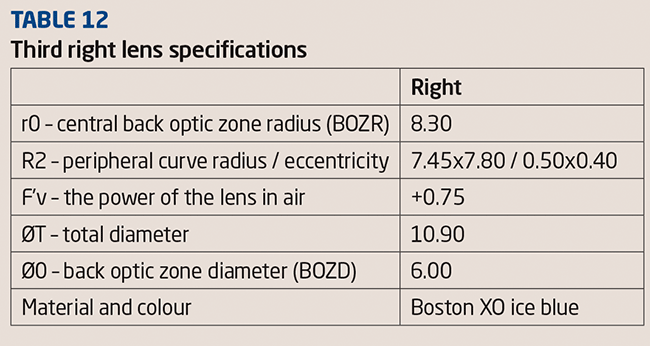
TP stopped wearing the right lens so the refraction and corneal shape could return to normal to enable us to order the new lens. After a week we repeated refraction and topography on the right eye. The refraction was unchanged from the initial measurement and the topography picture looked the same. This new information was sent to the supplier through its special software system and the new lens arrived within a week (Table 12).
On collection of the new toric ortho-k lens, the vision with the lens was 6/6 and the over-refraction plano. TP wore the lens for four nights before we did the first aftercare. However after two nights she reported that she felt her vision was already better than with the previous lens.
After four nights the unaided vision was 6/6 in the right eye with a refraction of +0.50 / -0.25 X 25 and visual acuity of 6/5. TP was pleased with her vision and stopped using daily disposable lenses during the day. She continued to wear the new right lens with the original left lens and had good unaided vision throughout the day with no additional correction required. After a month with the new lens we checked the vision, refraction and visual acuity and found that the right eye now had vision 6/5-2, refraction +0.25 / -0.25 X 20 and visual acuity 6/5.
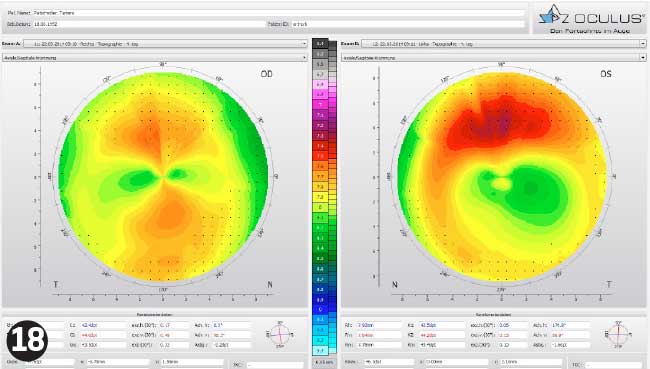
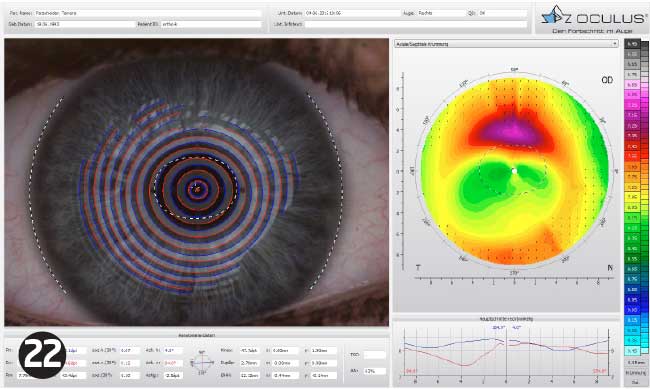
The topography pictures (Figures 18 to 22) show a slightly oval central zone due to the toric periphery. TP continued to wear the lenses and enjoyed being able to see in the morning on waking.
Case 3 — RB
RB was a 31-year-old sales assistant who wished to return to ortho-k after a period of wearing lenses on a daily basis. Prior to that he had worn ortho-k lenses for eight years. The spectacles he wore before he was fitted with his ortho-k lenses were -2.00DS R&L.
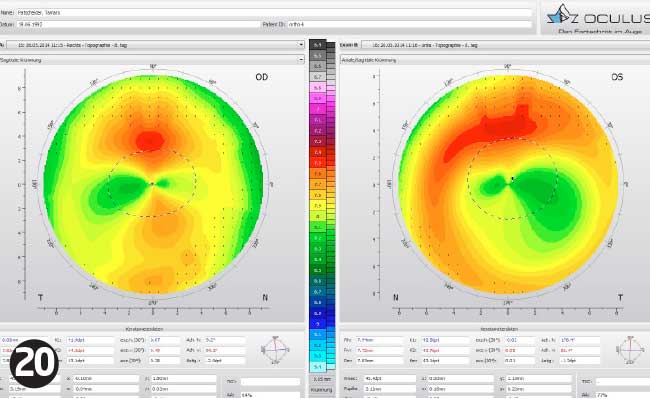
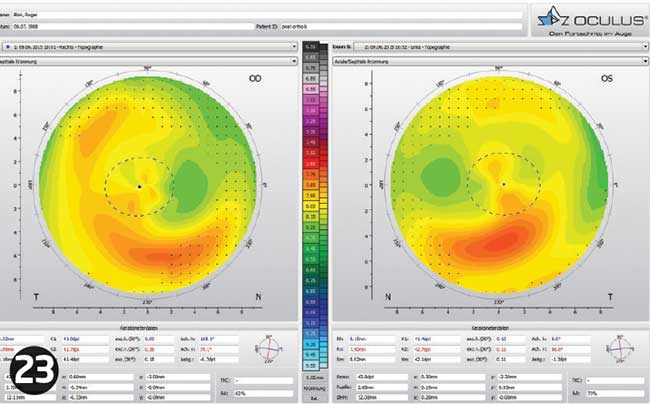
He first attended an appointment when he had not worn the lenses for two nights. His prescription had already started to return and his refraction was R -1.25/-0.50 X 155 L -1.00/-1.00 X 20. A topography picture was taken (Figure 23). I gave him some daily disposable lenses and booked another appointment for two days later.
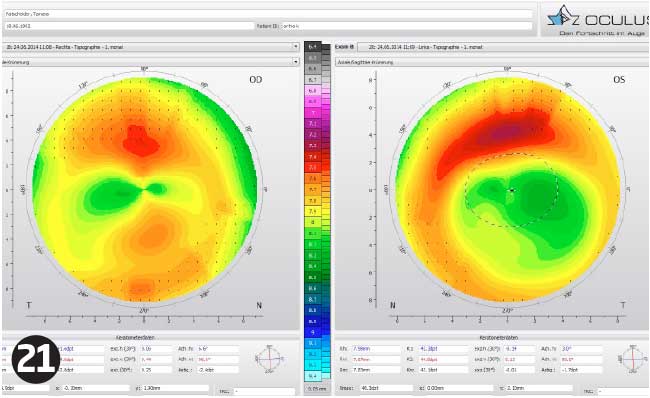
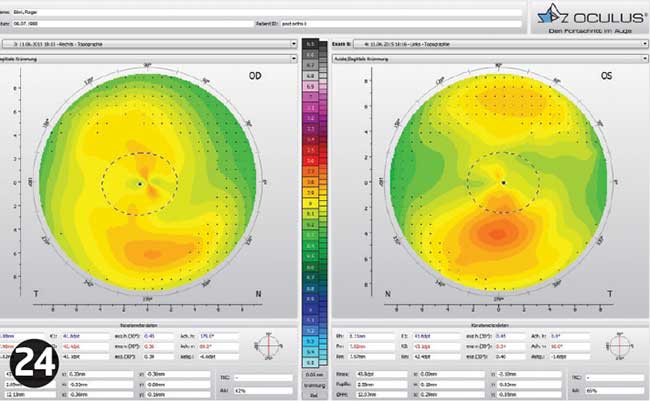
At the next appointment, after four days, his refraction had regressed further and was R -1.75/-0.50 X 175 L -1.75/-1.00 X 5. Topography was repeated (Figure 24). I felt at this point that most of his prescription had returned, but to be on the safe side we decided to do one final check after another five days.
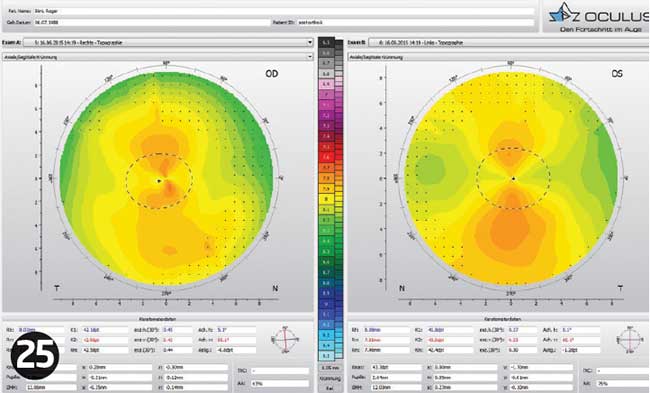
At this check-up the refraction had change slightly (R -2.00/-0.50 X 5 L -2.25/-1.00 X 180) as had the topography (Figure 25).
We felt it best at this point to fit RB with daily disposable lenses so he could wear them for a month to ensure the prescription remained stable. After four weeks he returned and, out of interest, we checked the prescription again and it remained unchanged. RB was then fitted with monthly disposable lenses and a follow-up appointment booked. RB now wears Biofinity R -2.25 L -2.25 /-0.75 180. He recently returned for a six-month lens check-up. His prescription is stable and he remains happy with his monthly disposable lenses.
Read more
An introduction to orthokeratology
Introduction to orthokeratology – lens collection and aftercare
Lisa Crouch is a UK-qualified optometrist practising at Visilab GlattzentrumSwitzerland. She specialises in orthokeratology and complex contact lens fitting