Accommodation is required to maintain clarity of an object at any distance closer than infinity. It is measurable in human babies from one month of age and becomes more accurate by six months.1 This ability gradually decreases with age and shows a steady decline becoming noticeable at about the age of 40, a process we all know as presbyopia. While accommodation is essential for clear vision in everyday life, it can affect the accuracy of determining refractive error. In some cases, to obtain meaningful results requires cycloplegia – paralysing the muscles controlling accommodation and causing a loss in ability to focus.
Anatomy and physiology of accommodation
The crystalline lens is a clear convex structure behind the iris in the posterior chamber of the eye. It is supported by the suspensory ligaments that attach to the ciliary muscle in a 360 degree arrangement. In its relaxed state, a normal (emmetropic) eye should be focused for six meters and beyond giving clear distance vision. The light rays from a distant object entering the eye are nearly parallel, after travelling through the refractive structures namely the cornea, aqueous, crystalline lens and vitreous before focusing on the retina. The ciliary muscles are relaxed, and the crystalline lens is in the most stretched out and flattest form, hence producing the least refractive power. Close objects have light rays that enter the eye in a divergent configuration therefore resulting in the image focusing behind the retinal plane and being blurred. The accommodative response causes a contraction of the ciliary muscle in an inward and anterior direction, relaxing the suspensory ligaments. The leads to a ‘fattening’ and hence more convex curvature of the lens that allows closer focus.2
Figure 1 Innervation of the eye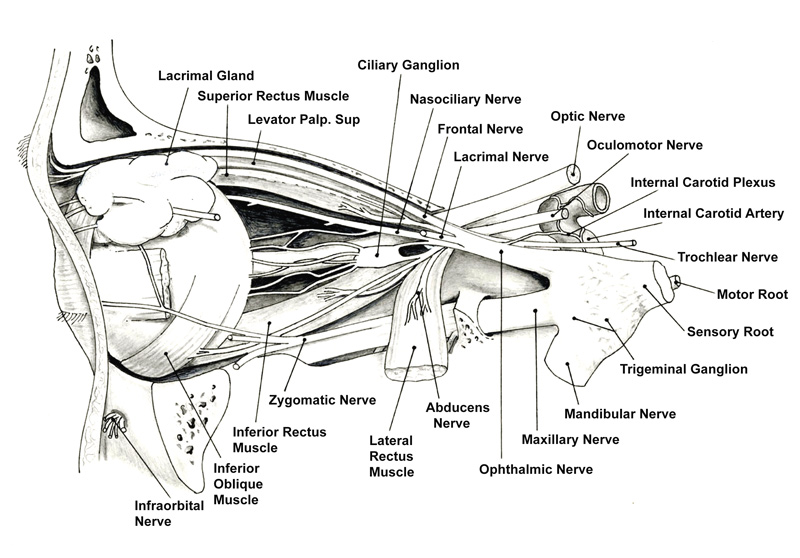
Accommodation is controlled by the parasympathetic system. The 3rd (oculomotor) cranial nerve originates from the central nervous system at the level of the midbrain (figure 1). Parasympathetic nerve fibres within the 3rd nerve then synapse at the ciliary ganglion. The neurotransmitter acetylcholine is made at the junction and released when an action potential arrives. This crosses the post synaptic cleft where it then reaches the receptors on the post synaptic membrane of the ganglion. A resulting chemical reaction causes depolarising of the neuronal membrane and an action potential is relayed along the nerve to the ciliary muscle in the eye. The receptors at the level of the ciliary body are muscarinic (figure 2). These are also true of those found in the iris sphincter, salivary glands and heart and bronchiolar nerves, the importance which will become relevant when considering drugs that affect these receptors.3
Figure 2 Flow chart showing the autonomic nervous supply of the eye and how it is influenced by different drugs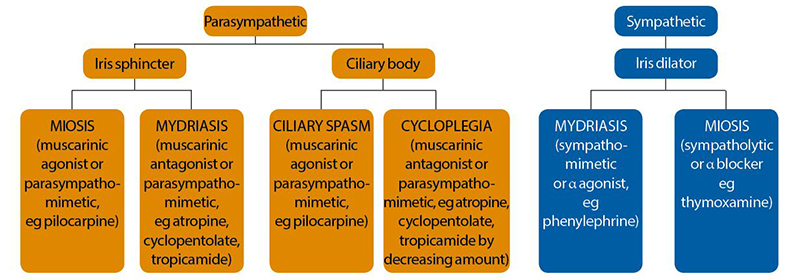
The triad of the accommodative response is accommodation, miosis and convergence. Pupil constriction aids the reduction of peripheral light rays which contribute to blurring and gives a greater depth of focus. The final component in the triad for clear near vision is convergence of the two eyes to allow bifoveal fixation.2
Cycloplegic drugs
Drugs that arrest accommodation, cycloplegics, are used routinely in optometric practice to aid refraction. The ideal cycloplegic drug should:
- Produce adequate cycloplegia
- Work in a short space of time
- Be reversible in a short time
- Not have any serious systemic or ocular side effects
- Be easy to administer
- Not be cost prohibitive
Generally, full cycloplegia is not required and residual accommodation of one to two dioptres is acceptable in most primary care cases. This outweighs the dangers of the potential side effects of an increased dose of more potent drugs (such as atropine) required for full cycloplegia.
The most commonly used cycloplegic drugs are anti-muscarinics. These molecules compete with acetylcholine and block the receptors to prevent nerve innervation. They also act on the iris sphincter muscle and produce pupil dilation. This side effect is sometimes useful for the fundal examination of children or uncooperative patients, although the associated photophobia is not often pleasant. Adult patients should be advised to avoid driving or operating machinery. Advising the child’s school that their vision will be blurred for several hours would also be useful. Systemic effects are possible in young children due to their low body weight and immature metabolism,4 therefore precaution advice must be given to the parent in case this effects occurs after they leave the practice.
A decrease in anterior angle drainage and raised intraocular pressure can occur with the use of anti-muscarinics. The loss of contraction of the ciliary muscle during accommodation which normally contributes to the aqueous flow, may also compound this effect. Fortunately, those disposed to this are at an age group that do not often need these drugs to aid refraction but cycloplegia should be avoided in those who have had closed angle glaucoma.3
Cycloplegics are also used in the treatment of anterior uveitis, blunt trauma, conjunctival and corneal lacerations5 and it is therefore important to question patients exactly what eye drops they are on when refracting to prevent misinterpreting results.
Commonly used cycloplegics drugs are listed in table 1. In the exemptions from Normal Supply Requirements of Human Medicine Regulations 2012, a list of medications that are prescription only (POM) can be sold or supplied to a GOC registered optometrist and may be used in the course of their professional practice. These are not to be supplied to the patient. Atropine can only be used and supplied by those with additional supply and independent prescriber status.
Cyclopentolate
This is the most commonly used cycloplegic drug and is readily available and appropriate for most cases requiring cycloplegia in primary care practice. It is available in the UK as 0.5 and 1% cyclopentolate hydrochloride in multidose bottles as Mydrilate (Intrapharm Laboratories Ltd) and single dose Minims (Bausch and Lomb UK Ltd) (figure 3). Its effect begins fairly rapidly, and the maximal effect can be reached in 20 to 40 minutes. Recovery can allow reading after four hours, although it can take 12 to 24 hours. Opinions as to which concentration to use varies among different authors. Half a percent is usually recommended for 12 to 16-year-olds3 and 1% for one to 11 years old.6 The College of Ophthalmologists’ guidelines recommend refraction after 30 minutes after instillation of 1 % for over age six months, and 0.5% for younger babies with suspected strabismus.7 Repeatability using 1% cyclopentolate after 30 minutes has been shown to be good in both inter and intra practitioner comparisons.8
Side effects include disturbances to the central nervous system including hallucinations, ataxia and babbling speech. These are fortunately rare and wear off after a few hours.
Tropicamide
For teenagers and adults, this may be enough to produce the full cycloplegic effect required for refraction and its effects wear off quicker than cyclopentolate. One percent with two drops at 15 minutes apart is recommended. Some argue that tropicamide produces too much residual accommodation, using push up measurements. However, objective measurements appear to show only 1 D of residual accommodation and is therefore acceptable in most cases.9,10
Atropine
Atropine is required when there is significant hypermetropia and esotropia, as the full cycloplegia result is needed before possible surgical intervention. Also in children with very dark irises, when cyclopentolate has been used and inadequate dilation for fundal examination and refraction results are inconclusive, atropine will be considered. It is available as atropine sulphate: eye drops, 1% (non-proprietary) and single dose Minims 1% atropine sulfate (Bausch & Lomb UK Ltd).6 These can be used and supplied by optometrists holding the additional independent prescribing qualification.
Table 1 Commonly used cycloplegic drugs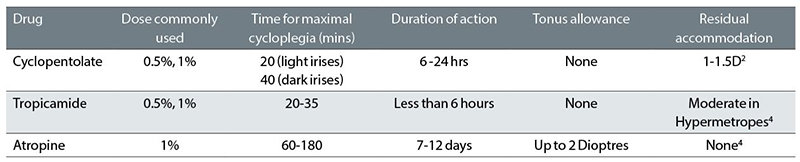
Many studies show repeated use of up to three drops of 1% cyclopentolate were as effective as 1% atropine, although how practical this would be in primary care practice needs to be a consideration.4 Atropine 1 % as an eye drop produces full cycloplegia after a few hours. However, the risk of systemic effects can be higher and atropine ointment instilled twice a day for three days before the refraction appointment is therefore often preferred. No ointment is used on the day of refraction as the oily residue may affect refraction results.4 It is not without risks and extreme caution should be exercised due to the risk of poisoning. This is a real risk as a small tube of atropine (3g) ingested accidently can cause death in a small child who can be seriously affected by as little as 10mg. Typical side effects seen include: rapid pulse, dry skin and mouth, excitement, respiratory paralysis.
How to use cycloplegic drugs
Before using cycloplegic eye drops, a full eye examination should be undertaken including a detailed history of any current medication (and possible interactions) or previous allergic reactions. A ‘dry’ retinoscopy result is also useful for prescribing purposes. In older patients, anterior chamber depth and tonometry should also be assessed. Warning about side effects should be given and consent from the patient or parent obtained to instil the drug.
It is recommended by some and used as standard protocol in clinical trials, to use 0.5% proxymetacaine to anaesthetise the cornea before instillation of cyclopentolate (figure 4). The advantages are that this may allow the patient to tolerate having the stinging drop in both eyes, especially in the second eye. Also, it improves the absorption rate of the cycloplegic drop. The disadvantages include the challenge of instilling more than one drop in each eye of less cooperative patients, the added cost and the possible inconvenience of needing to store proxymetacaine in refrigeration.
Placing drops on the medial canthus of uncooperative patients and then allowing the drop to fall into the eye on opening has been found to be as effective as instilling directly into the open eye.4 This method was also found to be more comfortable for the patient. Using a spray has also been found to be effective but is less readily available in UK. It has also been shown that instilling a smaller drop produces less blinking and reflex tearing, increasing the efficacy of the drop.11 This was more effective than closing the eyes after instillation or performing nasolacrimal occlusion.
Figure 3 Cyclopentolate Minims
In primary care, the standard drug of choice in over one-year-olds would be 1% cyclopentolate 1 drop and in light irises cycloplegia may be achieved in as little as 10 minutes.11 In dark irises at least 30 minutes is required before attempting refraction.11,12 For all iris colours, maximum cycloplegia is achieved after 40 minutes when residual accommodation is measured objectively. Greater amounts of residual accommodation are found in dark irises if measured subjectively.11 Mydriasis should not be used as an indicator for cycloplegia as although the onset is similar, full dilation can occur before full cycloplegia in light eyes. In dark eyes, cycloplegia can be reached before maximum dilation.11
Figure 4 The action of a topical cycloplegic may be enhanced by preinstillation
of a topical anaesthetic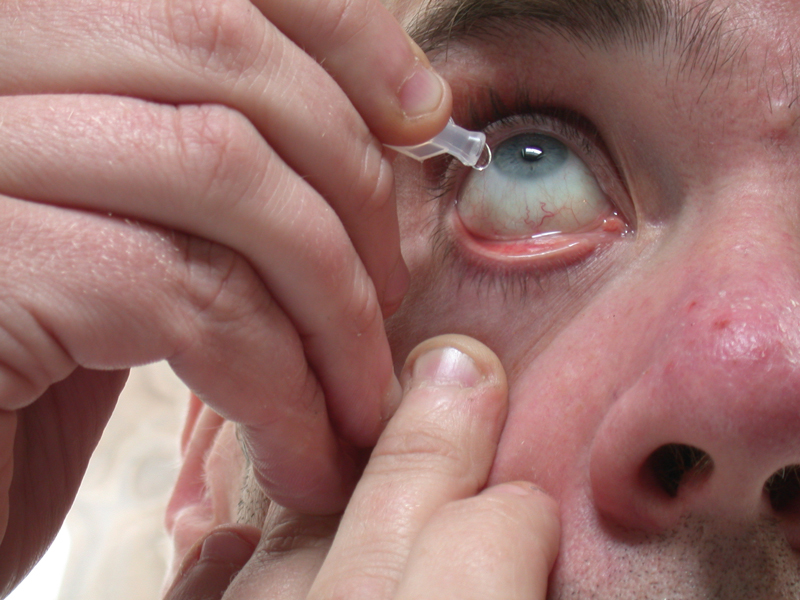
Determining when adequate cycloplegia is reached can be done in several ways. Measurement of residual accommodation in older patients, eg using a RAF ruler, can be performed with a +2.50DS in the trial frame and subtracting this amount after. Residual accommodation of 2D or less is considered acceptable.1 In younger patients, use of the retinoscopy reflex is required. Fluctuations of accommodation and hence a change in speed or direction of the retinoscopy reflex when asking patients to fix from distance to near would indicate inadequate cycloplegia. Usually waiting another 10 to 15 minutes is all that is required. Analysing the retinoscopy reflex should also just be concentrated on the central 4mm of the dilated pupil as the spherical aberration distorts the reflex. The patient’s fixation should be on a distant target if possible (to counter any residual accommodation) but the retinoscope light is workable as a target for younger patients, and gives the added advantage of being on the visual axis. Loose trial lenses are preferable to phoropters for younger children. Older patients can also have a subjective refraction bearing in mind that final VAs will be about two lines worse than best VA due to the mydriasis.
When to use cycloplegic drugs
Accurate refraction requires fixation to be on a distance target, eg 6m or beyond, such that the accommodation is relaxed. When accommodation occurs either during objective (retinoscopy) or subjective refraction, this will result in an over myopic or under hypermetropic result. Where there are fluctuations of accommodative effort, the end point of the refraction would also be variable. Therefore, any cases where distance fixation or controlling accommodation is not possible, a cycloplegic refraction should be considered. This would include those who are unable to cooperate due to their young age, language barriers, communication or learning difficulties.
Table 2 Signs and symptoms requiring a cycloplegic refraction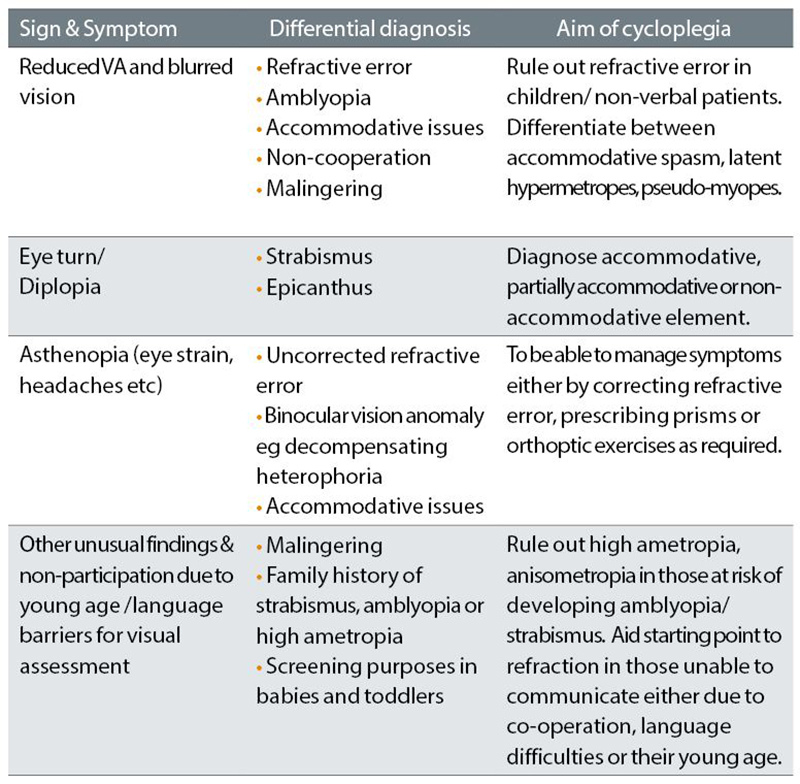
A cycloplegic refraction is useful to rule out any refractive error that would account for symptoms in those who are malingering. It is also useful for the diagnosis of many conditions listed, whose signs and symptoms are listed in table 2. A summary of patients requiring cycloplegic refractions would be:
- Bilateral or unilateral reduced visual acuity in child with unexplained cause
- Strabismus on first detection and possibly at annual review
- Non-verbal/communicative patients including very young children and babies
- Fluctuating retinoscopy reflex and reduced vision or VA
- Suspected latent hypermetropia/ pseudomyopia
- At first appointments at a hospital eye clinic
Prescribing tips
There are many opinions on prescribing and most practitioners will also rely on experience and judgement. Therefore, the following recommendations are based on recognised texts and the author’s own experience in community and hospital practice and may differ from other opinions.
Where there is a significant refractive error that is outside the norms for that age group, prescribing the refractive error found after cycloplegic refraction is a good line of first treatment. Visual acuities should be reviewed in six to eight weeks to check for improvement and monitoring at three to four monthly intervals until no further improvement is found before referring for amblyopia treatment.
In children with esotropia, full hypermetropia and astigmatism should be issued for full time wear. A review should then take place in six to eight weeks to see the effect of the spectacles. If it is a fully accommodative esotropia, ie it is eliminated by wearing the hypermetropic spectacles and the vision is improving, these can be monitored closely in the community at three to four monthly intervals there is any residual amblyopia that needs treatment.
In non-strabismics, correction of moderate hypermetropia may be reduced to help adaptation. A quarter or third off the cyclo result of the worst eye appears to be consistent with later subjective results. This will also depend on the presenting symptoms and uncorrected vision. If the VA is poor, consider correcting more of the refractive error to try and improve the VA. Correction of the difference in anisometropia should be maintained. For example, for a cyclo result R +3.00DS L +1.00DS, take a 1/3 off the stronger eye (+3.00DS) and prescribe R+2.00Ds L Plano. This seems to avoid ‘over plussing’ and causing reduced distance VA and appears to be similar to the natural non-cycloplegic state of the eyes. A subjective refraction either on the same day or on another visit – a ‘post-cyclo’ – would help the prescribing decision.
In the absence of any significant refractive error and reduced VA, in non-strabismics consider the following. In a young child, is the type of test appropriate? You may need to use pictures as well as letters or numbers. Late after-school appointments can result in tiredness and poor concentration for the tests. Sometimes, simply rechecking on an early Saturday morning visit produces dramatically improved vision results. In children with strabismus and no significant refractive error, routine referral to a hospital for amblyopia and possible surgical treatment may be appropriate.
The relationship between accommodation and accommodative convergence should also be remembered. When correcting hypermetropia, this relaxes accommodative convergence meaning the eyes may diverge. Measurements of heterophoria and heterotropia are therefore important before refraction to see the effect that the correction of the refractive error has on ocular motor balance. For a child with exophoria, correcting all their hypermetropia and relaxing their accommodative convergence may cause decompensation into an exotropia which is undesirable. The AC/A ratio (accommodative convergence produced by each dioptre of accommodation) is usually four prism dioptres to 1D. Therefore, any spherical adjustment to a prescription can be used to manipulate this to the advantage of controlling a convergent or divergent muscle imbalance. Reducing plus or increasing minus can produce convergence to aid exo deviations and vice versa. The amount increased or decreased would also depend on the VA being maintained and the amount of excessive accommodation required for comfortable vision. Usually no more than 1 to 1.5 D of manipulation can be tolerated. A cycloplegic refraction should be performed as a starting point before considering any refractive change. Also, measure the amplitude of accommodation to see if it will be adequate for this treatment.
One Hospital Paediatric Eye clinic’s view on cycloplegic refractions and prescribing
In the author’s place of work in a hospital paediatric eye clinic in Hertfordshire, we are very happy for children to be prescribed spectacles by the referring optometrist so they have the benefit of corrected refractive error during their wait for referral. We do recommend that a cycloplegic refraction be attempted as a minimum, even if co-operation is not good. Practitioners should have confidence in prescribing as it is rare that when we repeat the cycloplegic refraction, the results are found to be very different. In the absence of strabismus, VA should be measured after six to eight weeks after collecting spectacles. If the VAs are improving or normal, there is no need for referral to the hospital eye service. Cooperation and concentration can be better in the community where there is less waiting around than in a busy children’s clinic where the whole appointment can take up to two to three hours, to see an orthoptist, optometrist and doctor.
Case 1: Refraction results not expected with level of uncorrected vision
Symptoms:
A 14-year-old teenager complains of having intermittent blurred distance vision at school for the past month. This can occur at any time of day. Near vision appears fine. He has been revising long hours for his exams and loves his computer games in his spare time.
Findings:
Vision: R 6/7.6 L6/7.6 N5
Ret: R -2.50DS L-4.00DS (fluctuating reflex)
Subjective: R -1.75DS 6/6 L-2.00DS 6/6, N5.
Amplitude of accommodation R 5D L5D Bin 5.5D.
All other clinical findings including ocular motor balance are normal. A cycloplegic refraction was performed in view of the uncorrelated findings of uncorrected vision and amount of myopia found, the large difference between the retinoscopy and subjective results, as well as the reduced accommodation.
Cycloplegic refraction findings (1% cyclopentolate): R +0.25DS 6/9.5 L Plano/-0.25 x 180. 6/9.5.
Action: Suspected accommodative spasm causing pseudo myopia. If the ‘dry’ subjective had been prescribed this would have caused more symptoms as the patient would have to accommodate to see clearly. These cases need careful counselling to find the cause of the spasm, which might include stress, over use of close vision due to revision and not knowing the importance of taking regular breaks. The cycloplegic refraction helps to diagnose pseudomyopia to enable the correct management.
Case 2 – Unexplained reduced VA
Symptoms:
Blurred vision for past 12 months, vague history in a 20-year-old man. Currently unemployed. One episode of presumed optic neuritis in RE one year ago and seen in the hospital eye service when VA first dropped and now both eyes. Many routine investigations including electrophysiology findings inconclusive. Now very depressed due to reduced vision. Observed to be reading on mobile phone in waiting area.
Signs:
Vision: R 6/120 L 6/120 N4.8
Ret: R -2.00DS 6/120 L -2.25DS 6/60
Subjective R -2.00DS 6/60 L-2.25DS 6/60 N48.
Cycloplegic refraction was carried out as a baseline as no ocular pathology was found to account for the reduced VAs.
Ret R-1.50/-0.50 x180 6/7.6 L-2.00DS 6/6
Patient did not appear too surprised or pleased that his VA had improved with the new refraction. New spectacles were prescribed and the patient further monitored. This patient presented with the same grossly disproportionately reduced VAs on his follow up. Only when he was under cycloplegia again, could he read smaller lines. In conjunction with his ophthalmologist he was prescribed 1% cyclopentolate for possible accommodative spasm but on review three months later, he did not continue this as he felt it did not help.
This case demonstrates an unusual presentation where the pattern of vision, refractive error and expected result do not add up. The cycloplegic refraction does reassure the clinician the ocular structures and visual pathway are normal as the VAs are normal. It seems highly likely that this is a psychosomatic case where the cause lies in non-ocular factors. Referral for counselling or psychiatric assessment may be required.
Sosena Tang is an optometrist based in Hertfordshire. She works in an independent practice and for the East and North Herts NHS trust and is also a College Assessor and Examiner.
References
- Nelson, J. (1988) Visual development: acuity and binocularity. Optometry. Edition Edwards, K. & Llewellyn, R. Butterworth &Co.
- Marieb, E. (1992). The Special Senses. In ‘Human Anatomy and Physiology’. 2nd Edition. The Benjamin/Cummings Publishing Company, Inc. California.
- Vale, Janet. (1988) Drug Use in Optometry. Optometry. Edition Edwards, K. & Llewellyn, R. Butterworth &Co.
- Wickum, S. & Amos J. F. (2008). Cycloplegic Refraction, in ‘Clinical Ocular Pharmacology’ Edition Bartlett, J.D. and Jaanus, S. D., Butterworth-Heinemann, 5th Edition, P343-348.
- Onofrey, B.E., Skorin, J. L. and Holderman, N. R. (2011). Ocular Therapeutics Handbook – A Clinical Manual. 3rd edition. Wolters Kluwer Health.
- Optometrists formulary (The College of optometrists. www.college-optometrists.org)
- Royal college of Ophthalmologists guidelines (2012). https://www.rcophth.ac.uk/wp-content/uploads/2014/12/2012-SCI-250-Guidelines-for-Management-of-Strabismus-in-Childhood-2012.pdf
- McCullough, S.J., Doyle, L. and Saunders, K.J. (2016). Intra- and inter-examiner repeatability of cycloplegic retinoscopy among young children. Ophthalmic and Physiological Optics 37(1).
- Manny R.E., Hussein M, Scheiman M, et al. (2001) Tropicamide (1%): an effective cycloplegic agent for myopic children. Investigative Ophthalmological Vision Science 42:1728-1731.
- Yazdani, N , Sadeghi, R., Momeni-Moghaddam H., Zarifmahmoudi L. and Ehsaei, A. (2018) . Comparison of cyclopentolate versus tropicamide cycloplegia: A systematic review and meta-analysis. Journal of Optometry, 11(3) :135-143.
- Manny, R.E., Fern, K.D., Zervas, J., Cline, G.E., Scott, S.K., White, J.M. and Pass, A.F. (1993). 1% cyclopentolate hydrochloride: another look at the time course of cycloplegia using an objective measure of the accommodative response. Optometry and Vision Science 70(8): 651-665.
- Laojaroenwanit, S., Layanun, V,. Praneeprachachon, P . and Pukrushpan, P. (2016) Time of maximum cycloplegia after instillation of cyclopentolate 1% in children with brown irises. Clinical Ophthalmol. 10: 897–902.
